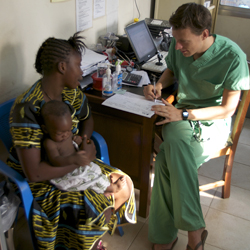
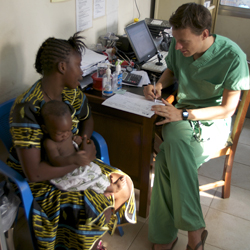
 FY2 Dr Mikey Bryant is in Sierra Leone with healthcare charity Mercy Ships. He has been volunteering in a children’s clinic for a year in a country where one in five children don’t live to see their 5th birthday. In this regular column he gives us an update on his experience.
FY2 Dr Mikey Bryant is in Sierra Leone with healthcare charity Mercy Ships. He has been volunteering in a children’s clinic for a year in a country where one in five children don’t live to see their 5th birthday. In this regular column he gives us an update on his experience.
“Quickly, hold this retractor!”
I grasp the rather small metal piece between my hands and pull it backwards, tightening the pressure on the skin. The underlying fat caves in around the retractor like quicksand around a child’s foot, and Karen sighs. She arrived here three weeks ago after her project with another NGO collapsed, and she has been become increasingly frustrated with our ever disappearing equipment, particularly large sized retractors.
Beloved of junior surgical doctors everywhere from Tasmania to Timbuktu, we were mystified at what they could possibly be used for – at least until I walked past a garage and found several of them holding up the back of a defunct looking bus, while men buzzed about changing the wheel. In spite of the obvious problems caused by the theft, I had to admire the innovation.
I am snapped out of my thoughts by Karen pushing the retractor out of the way and doing the rest of the procedure the old fashioned way, both hands delving deep inside the patient the way a hungry leopard tucks into a gazelle. Thankfully, she is far more skilled than I am, and we are soon pulling the baby’s head out through the uterine wall. Remarkably, the baby is crying almost straight away and we are looking at a healthy boy thrusting his arms out into the air and grabbing for his mother.
I have always been fascinated by obstetric surgery, especially the ability to put everything back after a long procedure involving more incisions than Jeremy Paxman on Newsnight. The whole bundle of organs seems to flow out like too many clothes from a suitcase, and I’m still in wonder as to how all the bowels get sandwiched back inside, leaving patients with such small scars.
A young girl, Kadijah, came to the clinic yesterday. She had been suffering from a high fever with vomiting for the previous three days, and had been to see the traditional healer, who had given her a mixture of green and yellow herbs, a concoction straight out of the jungle book. Unsurprisingly, her condition had not improved a great deal and by the time she had turned up at the clinic, I would have admitted her, had it not been for the family’s insistence that she should be treated at home. I had pleaded with the family to get to the clinic early today and get in ahead of the queues, and had been worried when she hadn’t turned up this morning.
Her family lead me to their home, a ramshackle lean-to held together with old pieces of rope and palm fronds, with no flooring to speak of. Inside, Kadijah is barely conscious, lying on a wooden cot covered by small pieces of material, curled up into a pale ball. Someone has put a drip in her arm, attached to a bag of fluid hanging from one of the palm branches. It takes me a few moments to work out what is wrong with this picture, until I see that the drip still has the needle attached, and most of the fluid is just dribbling onto the floor. Her Mum looks up at me blankly, and I ask her how Kadijah has been doing and why they didn’t come to the clinic this morning. Her only answer is to point at the drip, clearly believing this magic injection is the key to everything.
I try to pick up the conversation from where we left off yesterday, and try to talk the ominously calm parents into taking their child into hospital. I might as well be trying to run through quicksand, both parents are haunted by memories of their first child dying four years previously after a three day admission. Every time I mention going into hospital, there are floods of tears from Mum and torrents of angry defiance from Dad.
I feel utterly devastated, trapped by Sierra Leone’s limited of understanding of illness, while my own medical ethics and everything in me just wants to pick the child and sprint into the hospital, knowing we can probably still save her. There is no way that they will let me take her in, so all I can do is sort out the drip properly, get some more fluid to treat her with overnight and train the mother to check the pulse and temperature. I struggle not to feel too unwell as I leave the house, and wish there was more I could do to change the outcome.
The ethical struggles here are so much rawer; how far to push a family that essentially don’t trust Western medicine? When to cut our losses and give the family what they want? Am I setting up a precedent for more patients deciding to treat their children at home?